EYE DISEASES AND DISORDERS
Adie's Pupil: Adie’s pupil is a neurological disorder—a type of disease that affects the nervous system. With Adie’s pupil, there is an abnormal pupillary response to light. In most cases, it affects only one eye. The affected pupil is usually larger than normal and does not constrict as it should in the presence of bright light.

Age-Related Macular Degeneration: Macular degeneration causes loss in the centre of the field of vision. In dry macular degeneration, the centre of the retina deteriorates. With wet macular degeneration, leaky blood vessels grow under the retina. Blurred vision is a key symptom.

Albinism: The term albinism typically refers to oculocutaneous (ok-u-low-ku-TAY-nee-us) albinism (OCA) — a group of inherited disorders where there is little or no production of the pigment melanin. The type and amount of melanin your body produces determines the color of your skin, hair and eyes.

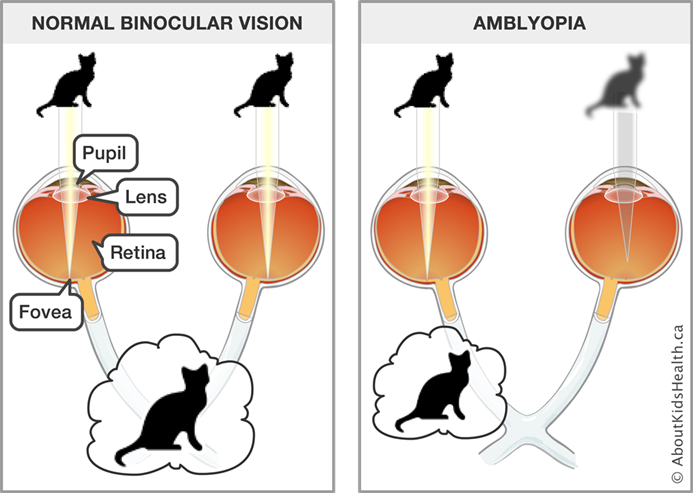
Amblyopia: Amblyopia occurs in early childhood. When nerve pathways between the brain and an eye aren't properly stimulated, the brain favours the other eye. The weaker — or lazy — eye often wanders inward or outward. Symptoms include a wandering eye, eyes that may not appear to work together or poor depth perception.
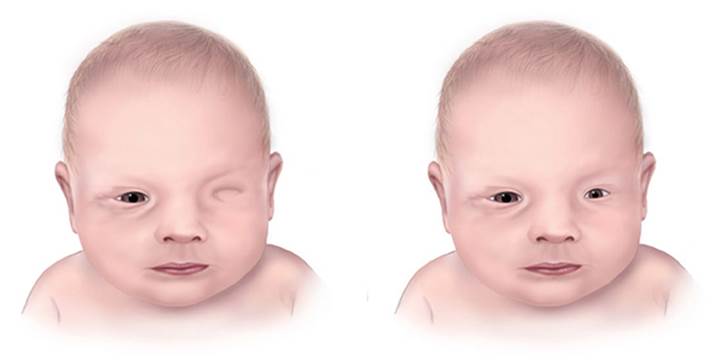
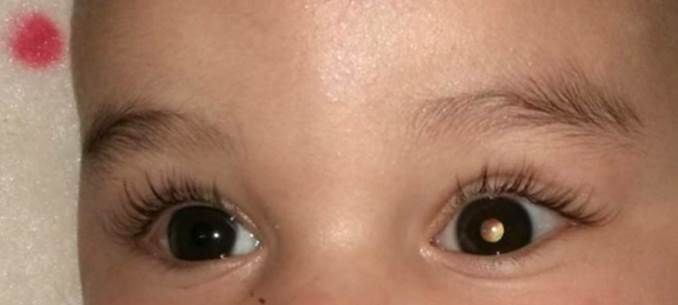
Anophthalmia / Microphthalmia: Anophthalmia and microphthalmia are birth defects of a baby’s eye(s). Anophthalmia is a birth defect where a baby is born without one or both eyes. Microphthalmia is a birth defect in which one or both eyes did not develop fully, so they are small.
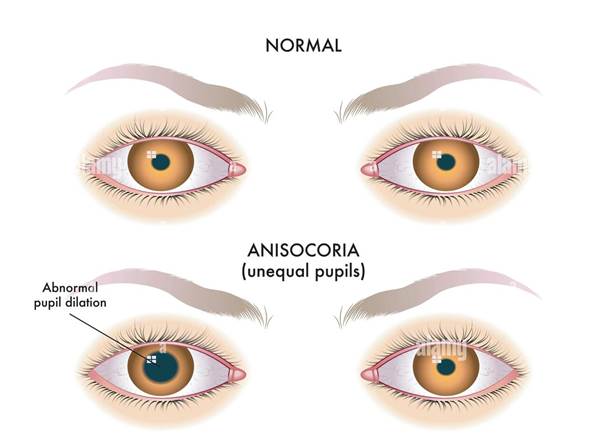
Anisocoria: Anisocoria is a condition characterized by unequal pupil sizes.
Aphakia: Aphakia means not having a lens inside your eye. The lens is the clear, oval-shaped structure behind the iris (colored part of your eye) and pupil. It focuses light rays on the retina. Without a lens, the eye is out of focus and vision is blurry.
Arcus Senilis: Arcus senilis is a half-circle of gray, white, or yellow deposits in the outer edge of your cornea, the clear outer layer on the front of your eye. It’s made of fat and cholesterol deposits. In older adults, arcus senilis is common and is usually caused by aging. In younger people, it may be related to high cholesterol levels. Arcus senilis is sometimes called corneal arcus.
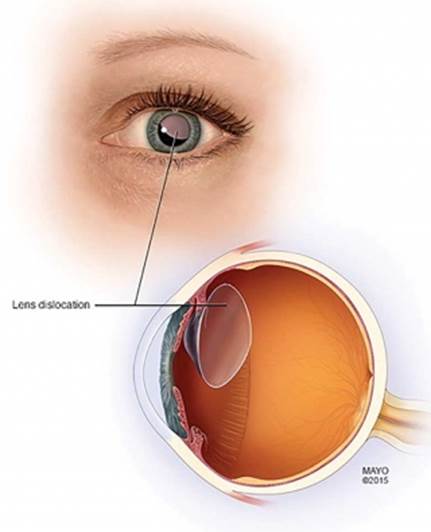
Astigmatism: Astigmatism is a common vision condition that causes blurred vision. It occurs when the cornea (the clear front cover of the eye) is irregularly shaped or sometimes because of the curvature of the lens inside the eye that prevents light from focusing properly on the retina, the light-sensitive surface at the back of the eye.
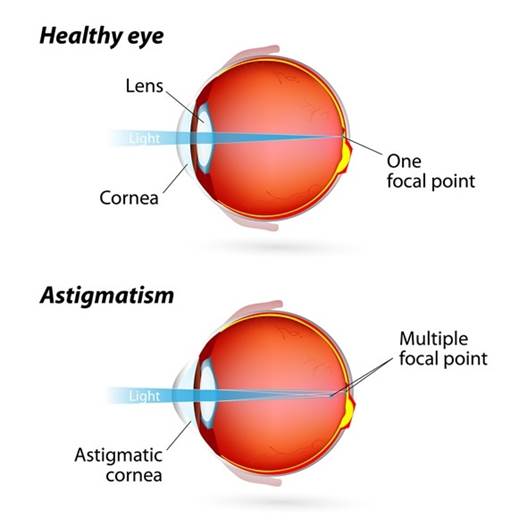
Bacterial Keratitis: Bacterial keratitis or corneal ulcer is an infection of the corneal tissue caused by varied bacterial species. It can be an acute, chronic, or transient infectious process of the cornea with a variable predilection for topographical, anatomical, or geographical domains of the cornea.
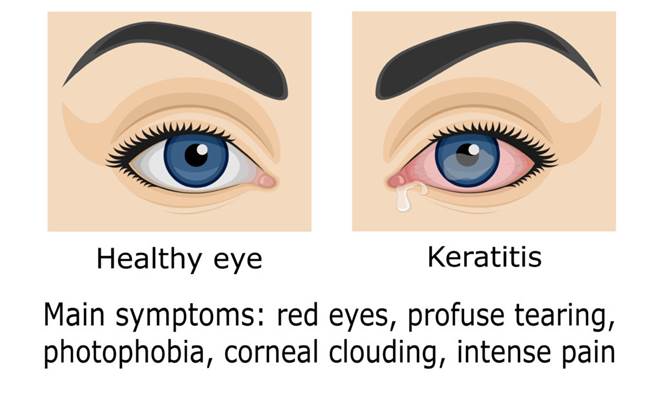
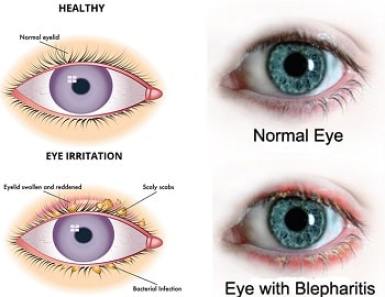
Blepharitis: Blepharitis commonly occurs when the tiny oil glands of the inner eyelid become inflamed. It often occurs along with other skin conditions or allergies. Symptoms include red, itchy eyelids that may look greasy and crusted. Dry eyes also are a symptom.
Branch Retinal Vein Occlusion (BRVO): Branch Retinal Vein Occlusion (BRVO) is a blockage of one or more branches of the central retinal vein, which runs through the optic nerve. Branch Retinal Vein Occlusion symptoms include: Peripheral vision loss. Blurred or distorted central vision.
Carotid Artery Disease: Carotid artery disease occurs when fatty deposits (plaques) clog the blood vessels that deliver blood to your brain and head (carotid arteries). The blockage increases your risk of stroke, a medical emergency that occurs when the blood supply to the brain is interrupted or seriously reduced.
Cataracts: A cataract develops when the lens in your eye, which is normally clear, becomes foggy.
For your eye to see, light passes through a clear lens. The lens is behind your iris (colored part of your eye). The lens focuses the light so that your brain and eye can work together to process information into a picture.
When a cataract clouds over the lens, your eye can’t focus light in the same way. This leads to blurry vision or other vision loss (trouble seeing). Your vision change depends on the cataract’s location and size.

Chalazia and Stye: Chalazia are enlargements of an oil gland (similar to a pimple) deep in the eyelid caused by an obstruction of the gland's opening. Styes are usually infected eyelash follicles. (inflammation of the edges of the eyelids). Some people may have one or two styes in a lifetime, but other people develop them repeatedly.

Charles Bonnet Syndrome: Charles Bonnet syndrome causes a person whose vision has started to deteriorate to see things that aren't real (hallucinations). The hallucinations may be simple patterns, or detailed images of events, people or places. They're only visual and don't involve hearing things or any other sensations.
Choroidal Neovascular Membranes: Choroidal neovascular membranes (CNVM) are new, damaging blood vessels that grow beneath the retina. These blood vessels grow in an area called the choroid. They break through the barrier between the choroid and the retina. When they leak or bleed in the retina they cause vision loss.
Coloboma: A coloboma is a congenital defect in the structure of either the eyelid or the eye. Coloboma of the iris is a hole or defect of the iris of the eye. Most colobomas are present since birth (congenital).

Color Blindness: If you have color blindness, it means you see colors differently than most people. Most of the time, color blindness makes it hard to tell the difference between certain colors. Usually, color blindness runs in families. There's no cure, but special glasses and contact lenses can help.
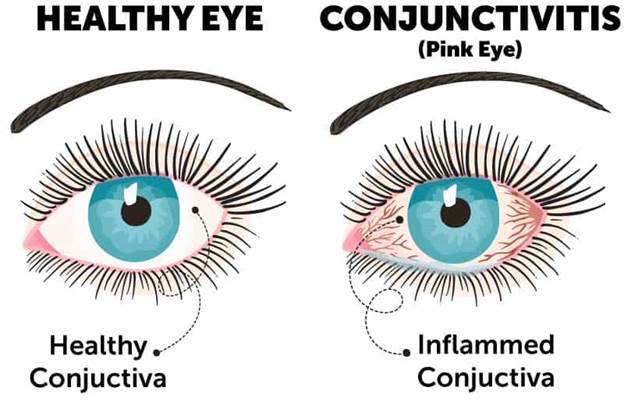
Conjunctivitis (Pink Eye): Conjunctivitis, or pink eye, is an irritation or inflammation of the conjunctiva, which covers the white part of the eyeball. It can be caused by allergies or a bacterial or viral infection. Conjunctivitis can be extremely contagious and is spread by contact with eye secretions from someone who is infected.
Symptoms include redness, itching and tearing of the eyes. It can also lead to discharge or crusting around the eyes.
Convergence Insufficiency: Convergence insufficiency (CI) is when the eyes have trouble working together while focusing on an object that is close by.
With normal vision, your eyes make a series of adjustments to work together to form a single image. When you look from an object that is far away to one that is close, the lens inside your eye slightly changes its shape. The dark circle inside the colored part of your eye (the pupil) gets smaller. Your eyes also move slightly toward the center (midline). This is called convergence. Your eye and brain carefully coordinate these changes. The result is that you can see a single, focused image. When you read, your eyes and brain also have to coordinate the quick, complex eye movements needed to scan a page.
If you have CI, your brain and eye may sometimes have trouble coordinating these changes. One of your eyes may sometimes turn out instead of converging toward the midline. This makes it hard for your eyes to work together. It can cause blurred vision, double vision, or eye strain. Or you may need to close one eye when reading.
CI is common. It may be slightly more common in women than in men
Corneal Abrasion: The cornea is the clear area in the center of the front of the eye. It is the part of the eye through which we see. When the cornea is scratched or scraped by a fingernail, contact lens, tree branch, or other object, the injury is called a corneal abrasion.
Corneal Dystrophies: Corneal dystrophies are a group of genetic, often progressive, eye disorders in which abnormal material often accumulates in the clear (transparent) outer layer of the eye (cornea). Corneal dystrophies may not cause symptoms (asymptomatic) in some individuals; in others they may cause significant vision impairment. The age of onset and specific symptoms vary among the different forms of corneal dystrophy. The disorders have some similar characteristics – most forms of corneal dystrophy affect both eyes (bilateral), progress slowly, do not affect other areas of the body, and tend to run in families. Most forms are inherited as autosomal dominant traits; a few are inherited as autosomal recessive traits.
Cytomegalovirus Retinitis: Cytomegalovirus retinitis. Cytomegalovirus (CMV) retinitis is a viral infection of the retina of the eye resulting in inflammation. Cytomegalovirus is a large herpes-type virus commonly found in humans that can cause serious infections in people with impaired immunity.
Detached Retina: Retinal detachment describes an emergency situation in which a critical layer of tissue (the retina) at the back of the eye pulls away from the layer of blood vessels that provides it with oxygen and nutrients. Retinal detachment is often accompanied by flashes and floaters in your vision.

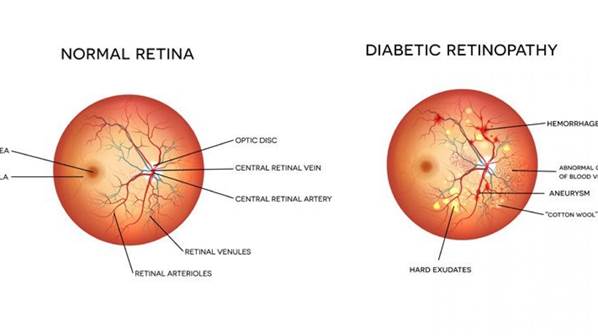
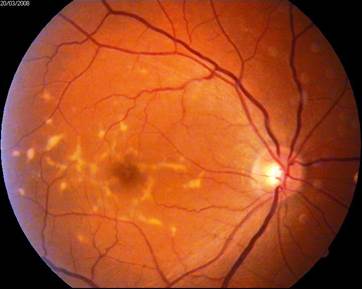
Diabetic Retinopathy: Diabetic retinopathy is a complication of diabetes, caused by high blood sugar levels damaging the back of the eye (retina). It can cause blindness if left undiagnosed and untreated.
Drusen: Drusen are small yellow deposits of fatty proteins (lipids) that accumulate under the retina.
The retina is a thin layer of tissue that lines the back of the inside of the eye, near the optic nerve. The optic nerve connects the eye to the brain. The retina contains light-sensing cells that are essential for vision.
Drusen are like tiny pebbles of debris that build up over time. There are two different types of drusen: soft and hard.
· “soft” drusen are large and cluster closer together
· “hard” drusen are smaller and more spread out
Having a few hard drusen is normal as you age. Most have at least one hard drusen. This type of drusen typically does not cause any problems and doesn’t require treatment.
Soft drusen, on the other hand, are associated with another common eye condition called age-related macular degeneration (AMD). It’s called “age-related” macular degeneration because it’s more common in people older than 60.
As soft drusen get larger, they can cause bleeding and scarring in the cells of the macula. Over time, AMD can result in central vision loss. In other words, the condition can affect what you’re able to see when you’re looking straight ahead.
Drusen can also occur in the optic nerve. Unlike drusen in the retina, optic nerve drusen can cause minor loss of peripheral (side) vision. Optic nerve drusen are not related to aging. They’re more commonly seen in children.
Dry Eye: Dry eye occurs when the eyes produce too few tears or the tears evaporate too quickly. The condition can affect one or both eyes. Possible symptoms include eye pain or discomfort, blurred vision, and increased sensitivity to light.
Ectropion: When part or all of the lower eyelid turns outwards away from the eye, the condition is known as an ectropion. There are various causes but the most common cause is an ageing effect of the eyelid that occurs in some older people. Someone looking at you might be able to see part of the pink inner surface of the affected eyelid.
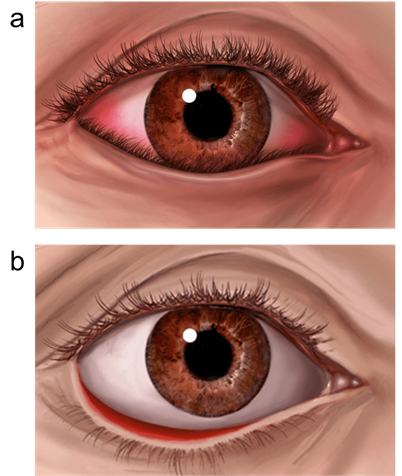
Entropion: Entropion (en-TROH-pee-on) is a condition in which your eyelid turns inward so that your eyelashes and skin rub against the eye surface. This causes irritation and discomfort. When you have entropion, your eyelid may be turned in all the time or only when you blink hard or squeeze your eyelids shut. Entropion is more common in older adults, and it generally affects only the lower eyelid.
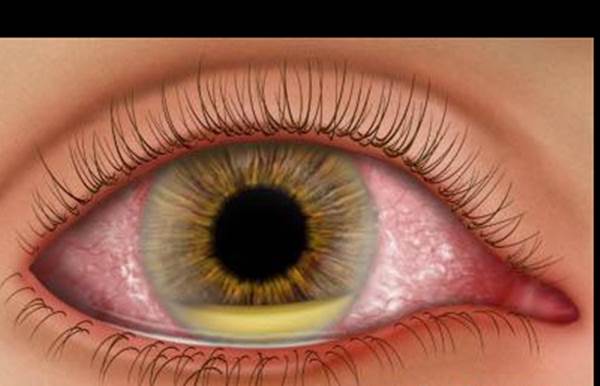
Endophthalmitis: Endophthalmitis is a purulent inflammation of the intraocular fluids (vitreous and aqueous) usually due to infection. Serious intraocular inflammatory disorder resulting from infection of the vitreous cavity. Progressive vitritis is the hallmark of any form of endophthalmitis.
Eyelid Spasm and Twitching: Eyelid twitches, or myokymia, can be caused by eye irritation, eye strain, lack of sleep, dry eyes, or too much caffeine. Severe or long lasting eyelid spasms may be a sign of other conditions. An eyelid twitch, or myokymia, is a repetitive, involuntary spasm of the eyelid muscles.
Farsightedness (hyperopia): Farsightedness (hyperopia) is a common vision defect that makes it difficult to focus on near objects. People with severe hyperopia can only focus on objects far away, or they cannot focus at all. People with farsightedness can see objects farther away better than closer objects. It occurs when the eyeball or the lens is too short or the cornea is too flat.
Fuchs’ Dystrophy: Fuchs’ endothelial dystrophy is a non-inflammatory, sporadic or autosomal dominant, dystrophy involving the endothelial layer of the cornea. Over the course of decades, the cornea develops guttae and increases in thickness, causing glare, halos, and reduced visual acuity. The damage to the cornea in Fuchs’ endothelial dystrophy can be so severe as to cause corneal blindness.
Fuchs’ dystrophy is often inherited in an autosomal dominant manner. This means if you have an inherited form of Fuchs’ endothelial dystrophy there is a 50% chance you will pass it on to your children. Spontaneous mutations in the genes for Fuchs’ dystrophy also can cause new Fuchs’ dystrophy in a person with no family history.
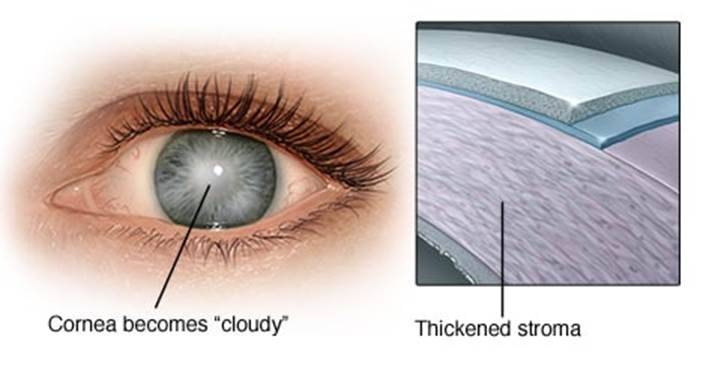
Fungal Keratitis: Fungal keratitis is an infection of the cornea (the clear dome covering the colored part of the eye) that is caused by a fungus. Some fungi that can cause fungal keratitis include:
· Fusarium species
· Aspergillus species
· Candida species
Glaucoma: Glaucoma is a condition in which fluid pressure rises within the eye. Without treatment, it can damage the optic nerve and lead to vision loss.
The front part of the eye contains a clear fluid, the aqueous humor. This fluid nourishes the eye and gives it its shape. The eye constantly produces this fluid and drains it away through a drainage system.
If a person has glaucoma, the fluid drains too slowly out of the eye. When this happens, fluid builds up, and pressure inside the eye rises

Open-angle glaucoma
Also known as chronic glaucoma, this is the most common type. It develops slowly, and a person may not notice any symptoms, even if slight vision loss occurs.
Many people with this type of glaucoma do not seek medical help until permanent damage has already occurred.
Closed-angle glaucoma
This is also known as acute angle-closure glaucoma. It can start suddenly with pain and rapid vision loss.
As the symptoms are noticeable, the individual will usually seek medical help, resulting in prompt treatment. This can prevent permanent damage.
Low-tension glaucoma
This is a rarer form of glaucoma in which eye pressure is not higher than the normal range but still causes damage that affects the optic nerve.
Experts know little about this condition, but it might be due to reduced blood supply to the optic nerve.
Pigmentary glaucoma
This is a type of open-angle glaucoma that typically develops during early or middle adulthood.
It involves changes in the pigment cells that give color to the iris. In pigmentary glaucoma, the pigment cells disperse throughout the eye.
If the cells build up in the channels that drain fluid from the eye, they can upset the normal flow of fluids in the eye. This can lead to a rise in eye pressure.
Childhood glaucoma
In rare cases, glaucoma can affect children due to genetic factors. The child may have:
· unusually large eyes
· excessing tearing
· cloudiness in the cornea
· sensitivity to light
Medication and surgery can help prevent vision loss.
Hemangioma: A hemangioma (he-man-jee-O-muh), known colloquially as a "strawberry mark", is a bright red birthmark that shows up at birth or in the first or second week of life. It looks like a rubbery bump and is made up of extra blood vessels in the skin. A hemangioma can occur anywhere on the body, but most commonly appears on the face, scalp, chest or back.

Herpes Keratitis: Herpetic keratitis is an infection of the cornea, the transparent front part of the eye, caused by the herpes simplex virus. While the herpes simplex virus that affects the genitals is type 2, the type that affects the eys and mouth is type 1.
This infection may affect the different layers of the cornea and cause an inflammatory reaction. It may also affect the most profound structures of the eye like the iris and cause inflammation inside the eye.
The cause of herpetic queratitis may also be the herpes zoster virus, commonly known as "shingles".
Heterochromia: Heterochromia is different colored eyes in the same person. Heterochromia is the presence of different colored eyes in the same person. Heterochromia in humans appears either as a hereditary trait unassociated with other disease, as a symptom of various syndromes or as the result of a trauma.
Hyphema: Hyphema is defined as accumulated red blood cells (RBC) in the anterior chamber of the eye. Blood must be grossly visible, either on direct inspection or slit-lamp examination. Blood accumulates from disruption of the vessels of the iris or ciliary body, usually due to trauma or underlying medical conditions. The anterior chamber is the area bounded by the cornea anteriorly, the angle laterally, and the lens and iris posteriorly. This space normally contains clear, aqueous humor, which is produced by the ciliary body and drained through the Canal of Schlemm. The angle, an important anatomic location, is where the trabecular network and the Canal of Schlemm are located. Blockage of this location inhibits aqueous drainage leading to an increase in intraocular pressure.

Idiopathic Intracranial Hypertension:
Idiopathic intracranial hypertension (IIH) happens when high pressure around the brain causes symptoms like vision changes and headaches. “Idiopathic” means the cause isn’t known, “intracranial” means in the skull, and “hypertension” means high pressure.
IIH happens when too much cerebrospinal fluid (CSF) — the fluid around the brain and spinal cord — builds up in your skull. This puts extra pressure on your brain and on the nerve in the back of your eye, called the optic nerve.
Iridocorneal Endothelial Syndrome: Iridocorneal endothelial (ICE) syndrome describes a group of eye diseases that are characterized by three main features: Visible changes in the iris (the colored part of the eye that regulates the amount of light entering the eye) Swelling of the cornea, and The development of glaucoma (a disease that can cause severe vision loss when normal fluid inside the eye cannot drain properly) ICE syndrome, is more common in women than men and is usually present in only one eye. The condition is actually a grouping of three closely linked conditions: Cogan-Reese syndrome; Chandler's syndrome; and essential (progressive) iris atrophy. The cause of ICE syndrome is unknown, however there is a theory that it is triggered by a virus that leads to swelling of the cornea.
Keratoconus: Keratoconus is characterized by the thinning of the cornea and irregularities of the cornea’s surface. The cornea is the clear, outer layer at the front of your eye. The middle layer is the thickest part of the cornea, mostly made up of water and a protein called collagen. Collagen makes the cornea strong and flexible, and helps keep its regular, round shape. This healthy cornea focuses light so you can see clearly. With keratoconus, the cornea thins and bulges into an irregular cone shape, resulting in vision loss.
Keratoconus generally begins at puberty and progresses into the mid-30s. There is no way to predict how quickly the disease will progress, or if it will progress at all. Keratoconus typically affects both eyes, with one being more severely affected than the other.

Lattice Degeneration: is a condition that involves abnormal thinning of the peripheral retina, which is the tissue that lines the back wall of the eye and is critical for maintaining good vision. When lattice degeneration is present, the retina is more vulnerable to developing tears, breaks, or holes that could ultimately lead to a visually debilitating condition called a retinal detachment. Clinically, lattice degeneration is characterized by oval or straight patches of thinned retina, sometimes accompanied by pigment clumps or a crosshatching pattern formed by sclerotic vessels. Lattice may be found in only one eye, but often is present in both. There may be just one lesion or clusters of many. Lattice is often located along the outer border of the retina.
Macular Edema: The macula is the part of the retina that helps us see fine detail, faraway objects, and color. Macular edema happens when abnormal fluid builds up in the macula, making it swell. It is typically caused by increased leakage from damaged retinal blood vessels or growth of abnormal blood vessels in the retina.

Macular Hole: A macular hole is a small break or hole in the central portion of the retina, called the macula. The macula is the central part of the retina which is responsible for distinguishing small details. Macular holes occur most frequently in healthy people and are most common in people in their 60s and 70s. Macular holes occur when the portion of the vitreous gel that lies on the macula spontaneously contracts, pulling some macula with it. When the pulling is strong enough, a hole can develop in the center, causing compromise of the loss of fine vision.
Macular Pucker: A macular pucker is an extra layer of tissue that has formed on the eye's macula. The macula is located in the center of the retina, an area of light-sensitive cells at the back of the eye. The macula is responsible for central vision, which is the sharp, straight-ahead vision we need for reading, driving, and seeing fine detail.
A macular pucker can cause blurred and distorted central vision. It is usually related to aging, and happens in people over age 50. Macular pucker is also called epiretinal membrane, preretinal membrane, cellophane maculopathy, retina wrinkle, surface wrinkling retinopathy, and premacular fibrosis.
Nearsightedness (Myopia): Nearsightedness, also known as myopia, is an eye condition that causes blurry distance vision. People who are nearsighted have more trouble seeing things that are far away (such as when driving) than things that are close up (such as when reading or using a computer). If it is not treated with corrective lenses or surgery, nearsightedness can lead to squinting, eyestrain, headaches, and significant visual impairment.
Nearsightedness usually begins in childhood or adolescence. It tends to worsen with age until adulthood, when it may stop getting worse (stabilize). In some people, nearsightedness improves in later adulthood.
For normal vision, light passes through the clear cornea at the front of the eye and is focused by the lens onto the surface of the retina which is the lining of the back of the eye that contains light-sensing cells. People who are nearsighted typically have eyeballs that are too long from front to back. As a result, light entering the eye is focused too far forward, in front of the retina instead of on its surface. It is this change that causes distant objects to appear blurry. The longer the eyeball is, the farther forward light rays will be focused and the more severely nearsighted a person will be.
Nystagmus: Nystagmus is a vision condition in which the eyes make repetitive, uncontrolled movements. These movements often result in reduced vision and depth perception and can affect balance and coordination. These involuntary eye movements can occur from side to side, up and down, or in a circular pattern. As a result, both eyes are unable to steadily view objects. People with nystagmus might nod and hold their heads in unusual positions to compensate for the condition. Generally, nystagmus is a symptom of another eye or medical problem. Fatigue and stress can make nystagmus worse. However, the exact cause is often unknown.

Optic Neuritis: Optic neuritis is a condition that affects the eye and your vision. It occurs when your optic nerve is inflamed.
The optic nerve sends messages from your eyes to your brain so that you can interpret visual images. When the optic nerve is irritated and inflamed, it doesn't carry messages to the brain as well, and you can't see clearly.
Optic neuritis can affect your vision and cause pain. When the nerve fibers become inflamed, the optic nerve can also start to swell. This swelling typically affects one eye, but can affect both at the same time.
Orbital Fracture: An orbital fracture is when there is a break in one of the bones surrounding the eyeball (called the orbit, or eye socket). Usually this kind of injury is caused by blunt force trauma, when something hits the eye very hard.
Photokeratitis: Photokeratitis, or Ultraviolet Keratitis, is a painful eye condition which can develop after unprotected exposure to Ultraviolet (UV) rays. Ultraviolet rays, from a variety of sources including welding arcs (arc eye, welder's eye) , reflections off snow (snow blindness), and germicidal UV lamps can damage the corneal epithelial cells and cause them to slough off after several hours. This is similar to having a "sunburn" of the eye. This leaves underlying corneal nerves exposed and damaged, causing symptoms of intense pain, photophobia, and foreign body sensation.
Pigment Dispersion Syndrome: Pigment-dispersion syndrome is an eye disorder that occurs when pigment granules that normally adhere to the back of the iris (the colored part of the eye) flake off into the clear fluid produced by the eye (aqueous humor). These pigment granules may flow towards the drainage canals of the eye, slowly clogging them and raising the pressure within the eye (intraocular pressure or IOP). This rise in eye pressure can cause damage to the optic nerve (the nerve in the back of the eye that carries visual images to the brain). If the optic nerve becomes damaged, Pigment-dispersion syndrome becomes pigmentary glaucoma. This happens in about 30% of cases. While men and women are affected in equal numbers, men develop pigmentary glaucoma up to 3 times more often than women.
Pinguecula and Pterygium: Pinguecula and pterygium are the common degenerations of the conjunctiva. A pinguecula is characterized by a yellowish raised growth on the conjunctiva typically at the nasal or temporal conjunctiva near the edge of cornea. Pterygium is the triangular shape of vascularized conjunctival tissue on the cornea and it invades the cornea (known as fibrovascular invasion of the cornea). Pterygium may start as a pinguecula that can remain small or grow large enough to cover some parts of the cornea. The body of a pterygium usually appears red with noticeable blood vessels. Redness depends on the growth of abnormal blood vessels. If it is left untreated, pterygium sometimes advances towards the center of the eye, affecting vision. They are not tumor. Generally, pinguecula and pterygium form in the corner of the eye near the nose. However, they may develop in the temporal of the eye and often both eyes are involved.
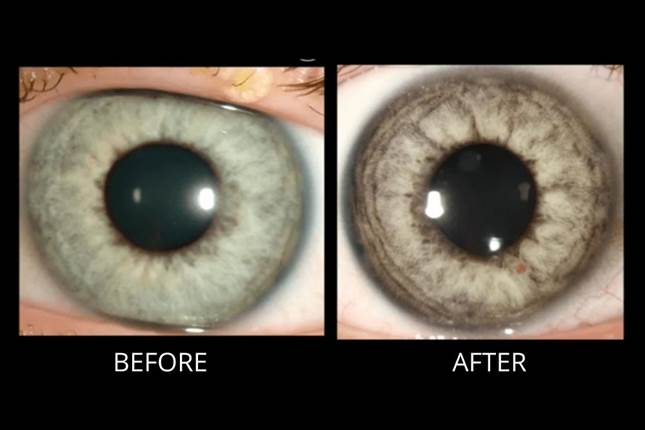
Posterior Vitreous Detachment: Posterior vitreous detachment (PVD) occurs when the gel that fills the eyeball separates from the retina. It's a natural, normal part of aging. PVD can cause floaters or flashes in your sight, which usually become less noticeable over time. The condition isn't painful, and it doesn't cause vision loss on its own.

Presbyopia: Presbyopia is the normal loss of near focusing ability that occurs with age. Most people begin to notice the effects of presbyopia sometime after age 40, when they start having trouble seeing small print clearly — including text messages on their phone.
Pseudoexfoliation Syndrome: Pseudoexfoliation syndrome
is a disorder in which flakes of material accumulates at the edge of the pupil, on the lens, in the drainage structures, and throughout other structures primarily in the front of the eye. When the eye’s drainage system is clogged by this flaky pseudoexfoliative material, as well as pigment, the eye pressure can increase and lead to pseudoexfoliation glaucoma. This syndrome refers to a condition that involves the entire body, but manifests primarily in the eyes.
Pseudostrabismus: Pseudostrabismus is when one or both of a child’s eyes look misaligned (crossed), but really they are not. This is unlike strabismus, when the eyes are misaligned, and point in different directions. With strabismus, one eye may look forward while the other eye turns in, out, up, or down. However, with pseudostrabismus, both eyes are pointing forward.
Pseudostrabismus is common in babies from birth to about 18 months old. A child can outgrow pseudostrabismus but not strabismus.
Ptosis: Eyelid drooping is excess sagging of the upper eyelid. The edge of the upper eyelid may be lower than it should be (ptosis) or there may be excess baggy skin in the upper eyelid (dermatochalasis). Eyelid drooping is often a combination of both conditions. The problem is also called ptosis.
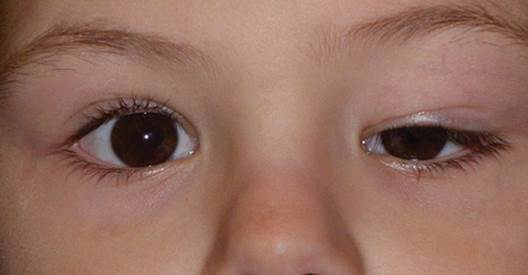
Retinitis Pigmentosa: Retinitis pigmentosa, also known as RP, refers to a group of inherited diseases causing retinal degeneration and a decline in vision. The retina is a thin piece of tissue lining the back of the eye. Rod and cone photoreceptors in the retina convert light into electrical signals that the brain interprets as vision. People with RP experience a gradual decline in their vision, because photoreceptors degenerate.
Forms of RP and related diseases include Usher syndrome, Leber congenital amaurosis, and Bardet-Biedl syndrome, among others.
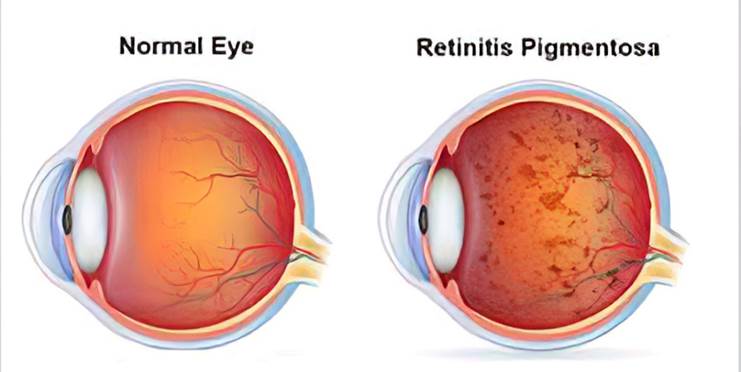
Retinoblastoma: Retinoblastoma is a cancer that starts in the retina, the very back part of the eye. It is the most common type of eye cancer in children. Rarely, children can have other kinds of eye cancer, such as medulloepithelioma, which is described briefly below, or ocular (eye) melanoma.
River Blindness (Onchocerciasis): Onchocerciasis, or river blindness, is a neglected tropical disease (NTD) caused by the parasitic worm Onchocerca volvulus. It is transmitted through repeated bites by blackflies of the genus Simulium. The disease is called river blindness because the blackfly that transmits the infection lives and breeds near fast-flowing streams and rivers, mostly near remote rural villages. The infection can result in visual impairment and sometimes blindness. Additionally, onchocerciasis can cause skin disease, including intense itching, rashes, or nodules under the skin.
Scleritis: Scleritis is the inflammation in the episcleral and scleral tissues with injection in both superficial and deep episcleral vessels. It may involve the cornea, adjacent episclera and the uvea and thus can be vision-threatening. Scleritis is often associated with an underlying systemic disease in up to 50% of patients.
Sjögren's Syndrome: Sjögren’s syndrome is a chronic disorder that causes insufficient moisture production in certain glands of the body, including the saliva-producing and tear-producing glands. The lungs, bowel and other organs are less often affected by Sjögren’s syndrome. Sjögren's syndrome is a lifelong autoimmune disorder that reduces the amount of moisture produced by glands in the eyes and mouth. It is named for Henrik Sjögren, a Swedish eye doctor who first described the condition. While dry mouth and dry eyes are the primary symptoms, most people who have these problems don't have Sjögren's syndrome. Dry mouth is also called xerostomia.
Stargardt Disease: Stargardt disease is a genetic condition caused by a tiny alteration in a single gene. It is also known as fundus flavimaculatus and is the most common form of macular dystrophy.
Stargardt causes a wasting of a central area of the retina called the macula. This area is eventually surrounded by a ring of white or yellow spots. An important layer of the retina, the retinal pigment epithelium (RPE), is also affected by an accumulation of ‘waste’ material called lipofuscin.

Stickler Syndrome: Stickler syndrome is a group of hereditary conditions characterized by a distinctive facial appearance, eye abnormalities, hearing loss, and joint problems. These signs and symptoms vary widely among affected individuals.
A characteristic feature of Stickler syndrome is a somewhat flattened facial appearance. This appearance results from underdeveloped bones in the middle of the face, including the cheekbones and the bridge of the nose. A particular group of physical features called Pierre Robin sequence is also common in people with Stickler syndrome.
Strabismus (Crossed Eyes): Strabismus (crossed eyes) is a condition in which the eyes do not line up with one another. In other words, one eye is turned in a direction that is different from the other eye.
Under normal conditions, the six muscles that control eye movement work together and point both eyes at the same direction. Patients with strabismus have problems with the control of eye movement and cannot keep normal ocular alignment (eye position).
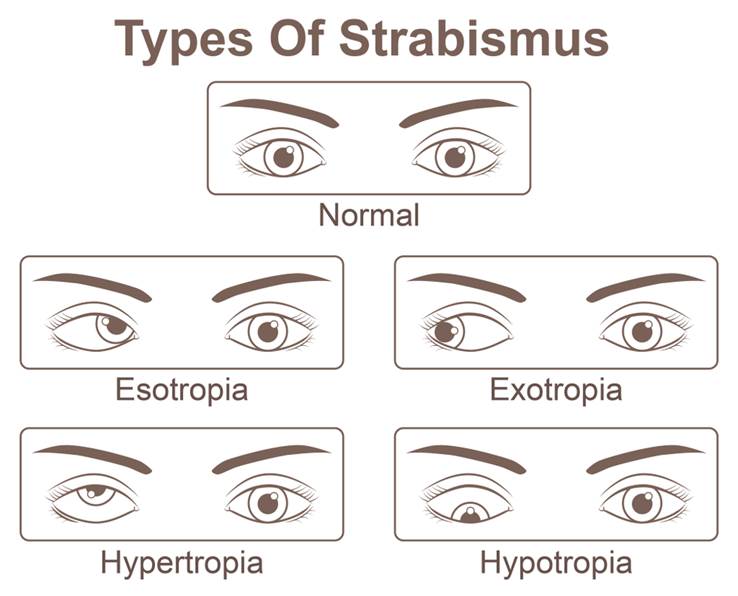
Strabismus can be categorized by the direction of the turned or misaligned eye:
· Inward turning (esotropia)
· Outward turning (exotropia)
· Upward turning (hypertropia)
· Downward turning (hypotropia)
Trachoma: Trachoma (truh-KOH-muh) is a bacterial infection that affects your eyes. It's caused by the bacterium Chlamydia trachomatis. Trachoma is contagious, spreading through contact with the eyes, eyelids, and nose or throat secretions of infected people. It can also be passed on by handling infected items, such as handkerchiefs.
At first, trachoma may cause mild itching and irritation of your eyes and eyelids. Then you may notice swollen eyelids and pus draining from the eyes. Untreated trachoma can lead to blindness.
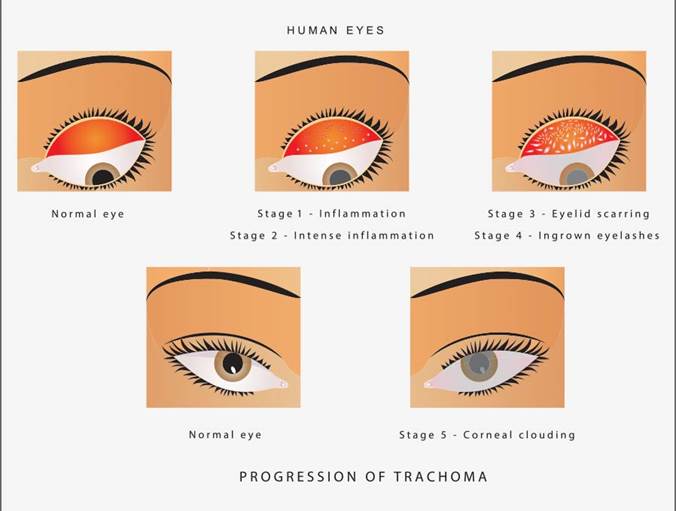
The World Health Organization (WHO) has identified five stages in the development of trachoma:
Inflammation — follicular. The early infection has five or more follicles — small bumps that contain lymphocytes, a type of white blood cell — visible with magnification on the inner surface of your upper eyelid (conjunctiva).
Inflammation — intense. In this stage, your eye is now highly infectious and becomes irritated, with a thickening or swelling of the upper eyelid.
Eyelid scarring. Repeated infections lead to scarring of the inner eyelid. The scars often appear as white lines when examined with magnification. Your eyelid may become distorted and may turn in (entropion).
In-turned eyelashes (trichiasis). The scarred inner lining of your eyelid continues to deform, causing your lashes to turn in so that they rub on and scratch the transparent outer surface of your eye (cornea).
Corneal clouding (opacity). The cornea becomes affected by an inflammation that is most commonly seen under your upper lid. Continuous inflammation compounded by scratching from the in-turned lashes leads to clouding of the cornea.
All the signs of trachoma are more severe in your upper lid than in your lower lid. Without intervention, a disease process that begins in childhood can continue to advance into adulthood.
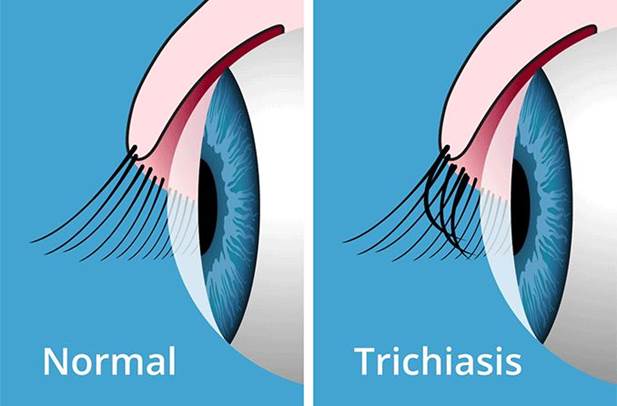
Trichiasis: Eyelashes serve several purposes for the human eye. They prevent dust and other foreign objects from entering the eye. They sense touch and thus aid in the protective blink reflex. And, they add to the cosmetic appeal of the human face and to the perception of beauty. In certain conditions, however, eyelashes can cause problems for and can even be dangerous to the eye. These conditions are called trichiasis and distichiasis.
Trichiasis is a condition of abnormal eyelash growth where the lashes are misdirected and grow inward toward the eye.
Distichiasis is a condition of abnormal eyelash growth where an extra set of lashes grows behind the normal lashes in the eyelid. These “extra” lashes also grow inward toward the eye.
In both trichiasis and distichiasis, lashes can reach the surface of and rub continuously or intermittently on the eye. These lashes are rough and disrupt the surface of the eye. This disruption can lead to problems ranging from mild discomfort and foreign body sensation to infection to permanent damage to the eye from scarring and vision loss.
Trichotillomania: Trichotillomania, also known as trich, is when someone cannot resist the urge to pull out their hair. They may pull out the hair on their head or in other places, such as their eyebrows or eyelashes. Trich is more common in teenagers and young adults.
Usher Syndrome: Usher syndrome is the most common genetic condition that affects both vision and hearing. The major symptoms of Usher syndrome are hearing loss and vision loss from an eye disorder called retinitis pigmentosa, or RP.
Uveitis: Uveitis (u-vee-I-tis) of the eye is inflammation inside the eye, specifically affecting one or more of the three parts of the eye that make up the uvea.
The uvea consists of the iris, the ciliary body and the choroid. The choroid is sandwiched between the retina and the sclera. The retina is located at the inside wall of the eye and the sclera is the outer white part of the eye wall. The uvea provides blood flow to the deep layers of the retina.
The type of uveitis you have depends on which part or parts of the eye are inflamed:
· Iritis (anterior uveitis) affects the front of your eye.
· Cyclitis (intermediate uveitis) affects the ciliary body.
· Choroiditis and retinitis (posterior uveitis) affect the back of your eye.
· Diffuse uveitis (panuveitis) occurs when all layers of the uvea are inflamed.
Vitreomacular Traction: The middle of the eye is filled with a substance called vitreous. In the healthy, young eye, this clear, gel-like substance is firmly attached to the retina and the macula by millions of microscopic fibers. As the eye ages, or as a result of eye disease, the vitreous shrinks and pulls away from the retina. The vitreous, over time, separates completely from the retina. This is called a posterior vitreous detachment (PVD) and is usually a normal part of aging. It happens to most people by age 70.
In some people with PVD, the vitreous doesn’t detach completely. Part of the vitreous remains stuck to the macula, at the center of the retina. The vitreous pulls and tugs on the macula, causing vitreomacular traction (VMT). This can damage the macula and cause vision loss if left untreated.
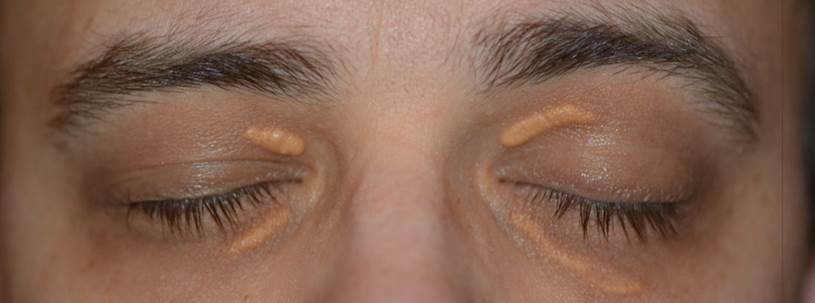
Xanthelasma: Xanthelasma (also known as xanthelasma palpebra) is a well-circumscribed flat or slightly elevated yellowish growth that typically occurs on or around the eyelids. It is made up of cholesterol deposits that accumulate underneath the skin and is usually an obvious clinical diagnosis. The lesions are not harmful and generally are not painful or itchy.